CITE THIS WORK
Plaza Fernández A, Sánchez Tripiana M, Hallouch Toutouh S. Esophageal squamous cell carcinoma and Lynch Syndrome: a coincidental association. RAPD 2026;49(2):68-69. DOI: 10.37352/2026492.6
Introduction
Lynch syndrome is an autosomal dominant disorder caused by mutations in DNA repair genes, which predisposes individuals to an increased risk of neoplasms, primarily colorectal and endometrial cancers. Its association with squamous cell carcinoma of the esophagus is rare and not yet well established; we present a clinical case that highlights this possible correlation.
Clinical case
A 68-year-old patient with no history of substance abuse, a history of endometrial carcinoma treated at age 55 and currently disease-free, was evaluated for de novo constitutional syndrome. A computed tomography (CT) scan was performed, revealing a pancreatic neoplasm that was unresectable due to vascular involvement (Figure 1). Subsequently, an endoscopic ultrasound with fine-needle aspiration (FNA) biopsy was performed, and histological analysis was consistent with squamous cell carcinoma. Given the rare nature of this neoplasm, the case was presented to a multidisciplinary committee, where a possible pancreatic metastasis from an occult squamous cell carcinoma was proposed. A positron emission tomography-computed tomography (PET-CT) scan was requested, which revealed a hypermetabolic lesion in the distal esophagus; biopsy confirmed primary esophageal squamous cell carcinoma with microsatellite instability. Genetic testing was requested, revealing a pathogenic mutation in the PMS2 gene, which confirmed the diagnosis of Lynch syndrome.
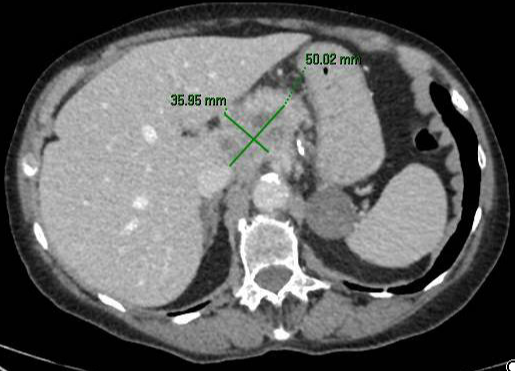
Figure 1
A heterogeneous lesion originating from the pancreas, without associated dilation of the bile duct or the duct of Wirsung, which completely encases the proximal third of the branches of the celiac trunk and the origin of the superior mesenteric artery, and comes into contact with the portal vein over an angle of >180°.
Discussion
Lynch syndrome is the most common cause of hereditary colorectal cancer and is associated with an increased risk of developing other cancers, such as those of the endometrium, stomach, pancreas, urinary tract, and ovary[1]. However, the association between Lynch syndrome and squamous cell carcinoma of the esophagus is rare and has not yet been fully documented[2],[3].
Squamous cell carcinoma of the esophagus is primarily associated with environmental factors such as tobacco and alcohol use, or chronic esophagitis. Nevertheless, some studies suggest a possible link to alterations in DNA repair mechanisms. In this context, the presence of mutations in PMS2, as in the case presented, could indicate an additional underlying mechanism that promotes esophageal carcinogenesis[2],[3].
Although the association between Lynch syndrome and esophageal squamous cell carcinoma remains uncertain, this case underscores the importance of considering less common neoplasms in the context of hereditary cancer predisposition syndromes. Likewise, the early identification of criteria suggestive of hereditary cancer and the performance of genetic testing facilitate better risk stratification and appropriate follow-up, which positively impacts the management of the patient and their family members[1].

 Descargar número completo
Descargar número completo Download full issue
Download full issue