CITE THIS WORK
Rodríguez Mateu A, Plaza Fernández A, Fernández Carrasco M, Fernández Muñóz LR. Upper gastrointestinal bleeding secondary to gastric varices due to segmental portal hypertension after Warshaw-type distal pancreatectomy. RAPD 2026;49(1):22-24. DOI: 10.37352/2026491.3
Introduction
Warshaw-type distal pancreatectomy with spleen preservation is a widely used surgical alternative for resection of the pancreatic body and tail in benign lesions or those with low malignant potential. This technique is characterized by ligation of the splenic artery and vein, maintaining spleen viability through collateral circulation from the short gastric vessels and the left gastroepiploic artery.
Its main appeal lies in its technical simplicity, especially in laparoscopic or robotic approaches, and in its usefulness when preservation of the splenic axis is not possible due to tumor proximity or adhesions, thus differentiating it from the Kimura technique.
Although the procedure has a high safety profile, it may be associated with specific vascular complications resulting from the interruption of splenic drainage, such as splenic infarction or the appearance of gastric varices secondary to segmental portal hypertension. Although these findings are usually subclinical, in a minority of patients they can progress to upper gastrointestinal bleeding.
We present the case of a woman with a history of distal Warshaw-type pancreatectomy who presented with an episode of gastrointestinal bleeding secondary to gastric varices.
Clinical case
A 38-year-old woman with a history of distal Warshaw pancreatectomy performed 15 years ago for mesenteric fibromatosis. She currently attends the emergency department after presenting with an episode of hematemesis accompanied by transient loss of consciousness. On arrival, she was found to have severe anemia (Hb 7.1 g/dL) and a tendency to hypotension, and an urgent transfusion of two red blood cell concentrates was initiated. Other notable laboratory findings included moderate thrombocytopenia (45,000/mm3).
Initial endoscopy revealed a large clot occupying the gastric fundus, with no clear bleeding point identifiable. Gastroscopy was repeated later, revealing markedly thickened gastric folds and a small fibrinous area consistent with gastric varices, which presented bleeding during the examination, leading to the administration of cyanoacrylate, after which the patient remained stable.
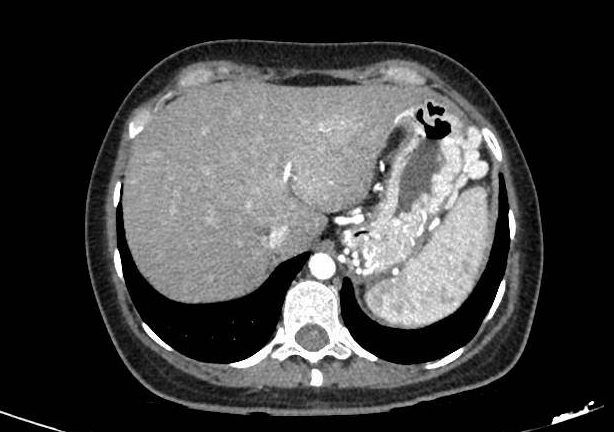
An urgent abdominal CT angiogram confirmed the presence of large varices in the fundus and perisplenic region, abundant collateral circulation, and splenomegaly, in the context of an absence of major splenic vessels, all consistent with left portal hypertension secondary to previous surgery (Figuras 1 y 2).
During admission, the patient remains stable and does not present any new bleeding episodes. She completes five days of somatostatin infusion, carvedilol is initiated at a dose of 6.25 mg every 12 hours as secondary prophylaxis, and intravenous iron is administered to treat anemia.
As definitive treatment, after joint assessment with the General Surgery and Interventional Radiology departments, the possibility of hepatic artery embolization is ruled out due to the post-surgical anatomical characteristics and the high risk of gastric ischemia in case of access through other branches. Finally, a scheduled splenectomy was indicated, which was performed without intraoperative incidents and with good subsequent evolution without new episodes of bleeding.
Discussion
Warshaw-type distal pancreatectomy allows preservation of the spleen by ligating the main splenic vessels and maintaining perfusion through the short gastric vessels and the left gastroepiploic artery. Although it is considered a safe and advantageous technique in benign or low-risk lesions, this forced redistribution of splenic drainage can cause significant hemodynamic alterations. The most relevant is left (sinistral) portal hypertension, a direct consequence of the interruption or occlusion of the splenic vein. This phenomenon causes splenic congestion and the development of a network of venous collaterals that drain preferentially into the short gastric vessels and the left gastroepiploic vein.
The formation of gastric varices is a classic manifestation of this hypertensive collateral circulation. Although up to a quarter of patients undergoing this technique may develop radiological perigastric varices, most remain asymptomatic. However, in a minority of cases, these varices can progress to rupture, leading to potentially serious upper gastrointestinal bleeding, which is more common in young patients with particularly strong collateral development.
The clinical picture usually manifests as hematemesis, melena, or acute anemia, and may be associated with shock in severe cases. Emergency endoscopy is the initial tool for identifying the cause of bleeding, along with imaging techniques (abdominal CT angiography and Doppler study), which are essential for confirming left portal hypertension, visualizing collateral circulation, and ruling out complications such as splenic infarction.
Acute management follows the general principles of variceal bleeding treatment: hemodynamic stabilization, prophylactic antibiotics, and splanchnic vasoconstrictor drugs such as somatostatin. The endoscopic treatment of choice for gastric varices is cyanoacrylate injection, while elastic ligation is reserved, with greater efficacy, for esophageal varices.
In scenarios where bleeding is refractory or anatomy prevents effective endoscopic or radiological procedures, splenectomy becomes the definitive treatment as it immediately corrects the pressure gradient and reduces the risk of rebleeding. It is also indicated in cases associated with splenic infarction, severe hypersplenism, or significant thrombocytopenia.
Optimal management of these patients requires a multidisciplinary approach, integrating gastroenterology, interventional radiology, and surgery. The therapeutic decision must be individualized, carefully assessing vascular anatomy, the extent of collaterals, and the options available at the center. Although the incidence of clinically significant bleeding after a Warshaw-type pancreatectomy is low, the potential severity of this event justifies a high index of suspicion in patients with a history of this technique who consult for gastrointestinal bleeding, even many years after the procedure.

 Descargar número completo
Descargar número completo Download full issue
Download full issue